What Does It Mean to Be a Nurse?
The nursing profession is a unique and multifaceted discipline that combines both art and science. At the core of nursing lies a deep respect for human dignity and an intuition for patients’ needs. Nurses have a rigorous educational foundation, which allows them to develop the necessary skills and knowledge to provide comprehensive care for their patients, as well as fostering empathy and communication skills essential for forming meaningful relationships with patients and their families.
Nursing is not only about providing medical care; it is also about promoting and restoring health, preventing illness, and supporting individuals and communities. Nurses collaborate with other healthcare professionals to ensure patient-centered, holistic care is provided efficiently and effectively. With over 80 specialties available for a professional nurse to choose from, the nursing field offers diverse career paths, allowing individuals to align their personal passions and strengths with their chosen specialty.
In summary, being a nurse encompasses the combination of various skills, knowledge, and qualities that enable them to provide exceptional care to patients. The nursing profession is dynamic and constantly evolving, making it an essential and respected component of the healthcare system.
The Role of a Nurse
Clinical Care
A nurse’s main responsibility is providing clinical care to patients. This involves managing patients’ physical needs, administering medication, and closely monitoring their vital signs. Nurses also perform various medical procedures, such as starting IV lines, administering injections, and providing wound care. The nurse-to-patient ratio can vary depending on the setting, like in an inpatient mental health unit where it’s typically 9 to 12 patients per nurse.
Patient Advocacy
Nurses play a critical role in patient advocacy. They serve as a bridge between patients, their families, and the healthcare team, ensuring that patients’ voices are heard and their rights are respected. This may include advocating for appropriate treatments, addressing concerns, and supporting patients’ decisions. Nurses also help patients navigate the often complex healthcare system.
Health Education
Educating patients about their health conditions and how to manage them is another important role for nurses. They provide health education by teaching patients about medication, proper nutrition, exercise, and other self-care strategies. Health education may also extend to disease prevention and maintaining overall wellness. Nurses can specialize in various aspects of patient care with over 80 specialties available in the nursing profession.
By fulfilling these roles, nurses demonstrate their commitment to delivering high-quality care, advocating for patients, and promoting health education throughout their communities.
Skills and Qualities
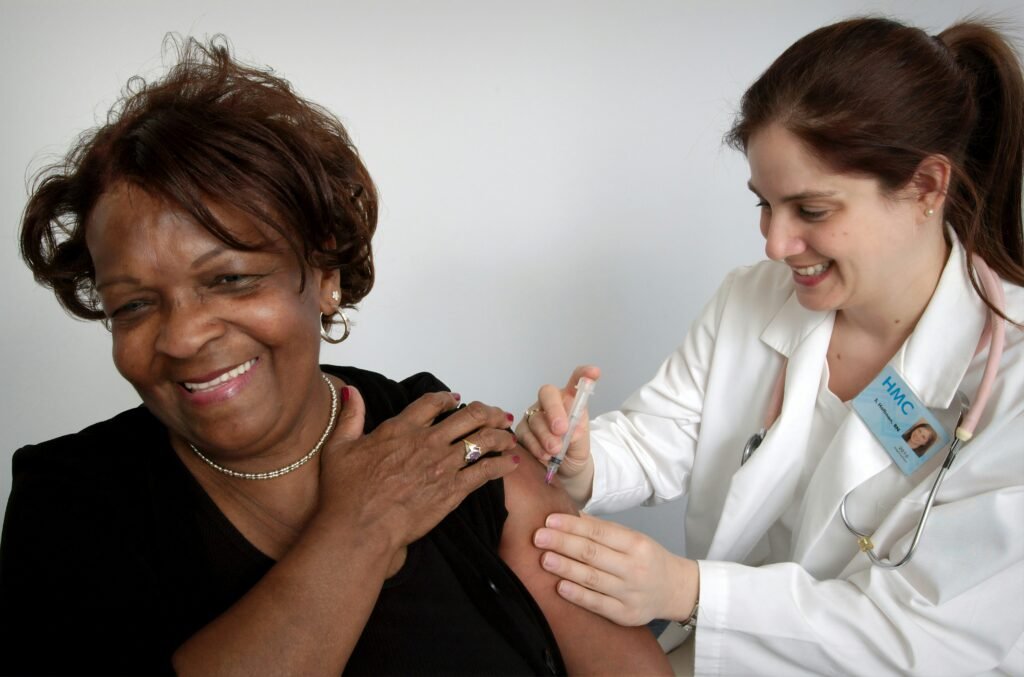
Nursing is a profession that requires a unique set of skills and qualities. In this section, we will discuss four essential qualities of a good nurse: Compassion and Empathy, Communication, Critical Thinking, and Adaptability.
Compassion and Empathy
One of the most important qualities of a good nurse is the ability to show compassion and empathy towards their patients. Compassion means showing kindness and understanding to others while empathy allows a nurse to put themselves in their patient’s shoes, understanding their emotions and needs. Nurses with these qualities tend to provide better patient-centered care and make the patients feel more comfortable during difficult times.
Communication
Effective communication is vital in nursing as it helps to reduce miscommunication and medical errors. Nurses must be able to clearly convey information to patients, their families, and other healthcare professionals to ensure proper care is provided. Cultural awareness is also an important aspect of communication, as it helps nurses understand diverse patient populations and improve overall patient outcomes.
Critical Thinking
Nurses often face complex situations that require strong critical thinking skills. They must be able to assess a patient’s condition, analyze data, and make informed decisions on the best course of action. Nurses who possess critical thinking skills are better equipped to provide appropriate and timely care, thus improving patient outcomes.
Adaptability
The healthcare industry is constantly evolving due to technological advancements and new scientific discoveries. Nurses need to be adaptable and willing to learn and grow to keep up with these changes. An ability to adapt to new situations, embrace change, and continuously update their skills is crucial for continued success in the nursing profession.
In summary, possessing qualities such as compassion, empathy, strong communication, critical thinking, and adaptability are important for being a successful nurse. Developing and honing these skills will not only improve patient care but also contribute to personal and professional growth in the ever-changing healthcare industry.
Professional Responsibilities
Adhering to Ethical Standards
Nurses hold a vital role in the healthcare system and are expected to follow a set of ethical standards. These principles focus on patient care, collaboration with other medical professionals, integrity, morals, and effectuating social change. Nurses’ commitment to ethical standards is crucial in safeguarding their patients’ well-being and upholding the reputation of the nursing profession.
Maintaining Patient Privacy
One key principle of nursing ethics is respecting and maintaining patient privacy. To protect the patients’ dignity, nurses should adhere to privacy regulations such as the Health Insurance Portability and Accountability Act (HIPAA). In practice, this entails:
- Securing patient records: Limiting access to patient information and ensuring proper disposal of documentation.
- Confidential communication: Discussing patient matters discreetly, without revealing personal information.
- Electronically safeguarding data: Utilizing secure messaging systems and protecting devices with strong passwords.
Continuing Education
Nursing is a vast profession, with over 80 specialties to choose from. To stay competent and current in their field, nurses must engage in continuing education efforts throughout their careers. This can involve:
- Maintaining licensure: Periodically renewing their nursing license as per the requirements of their respective states.
- Professional development: Pursuing certifications and advanced degrees to enhance their knowledge in a specific area.
- Staying informed: Keeping up-to-date with advancements in the nursing field, learning new techniques, and staying apprised of changes in healthcare policies.
By fulfilling these professional responsibilities, nurses contribute to enhancing patient care and promoting the overall integrity of the profession.
Types of Nursing

Registered Nurse (RN)
Registered Nurses play an essential role in providing healthcare, working in settings like hospitals, residential care facilities, or government offices. As an RN, individuals must meet specific educational requirements, such as obtaining a Bachelor of Science in Nursing (BSN) degree. The median salary for this profession is $77,600 annually, with a 9% projected job growth rate, which is about as fast as average.
Responsibilities of an RN include assessing patients’ health, creating care plans, administering medications, and performing vital healthcare procedures. They also collaborate with other healthcare professionals to ensure that patients receive the best possible care.
Licensed Practical Nurse (LPN)
An LPN, also known as a Licensed Vocational Nurse (LVN) in some states, is a nursing professional who provides essential patient care under the supervision of a registered nurse or a physician. LPNs typically complete a state-approved practical nursing program. These programs generally require one year of study and often lead to a diploma or certificate.
Some of the key tasks performed by LPNs include monitoring patients, assisting with personal care, administering prescribed medications, and performing basic nursing procedures. LPNs can work in various healthcare settings, such as hospitals, nursing homes, and clinics.
Advanced Practice Registered Nurse (APRN)
Advanced Practice Registered Nurses are highly educated and specialized medical professionals with a Master’s degree or higher in nursing. There are several types of APRNs, such as Nurse Practitioners, Certified Nurse Midwives, Certified Registered Nurse Anesthetists, and Clinical Nurse Specialists.
APRNs are qualified to perform advanced medical procedures, diagnose and treat health conditions, and prescribe medications. They often work independently or in collaboration with physicians. The expanded scope of practice for APRNs allows them to provide more comprehensive and personalized care for patients in a wide range of healthcare settings.
In conclusion, nursing is a diverse field with various education levels and specialization opportunities. The different types of nursing offer unique roles and responsibilities, allowing individuals to choose a career path based on their interests, qualifications, and goals.
Work Environments
Hospitals
Nurses in hospitals work in various departments, such as emergency rooms, surgery, intensive care units, and pediatrics. They often collaborate with other healthcare professionals to provide patients with the best care possible. Hospitals can be fast-paced and stressful environments, requiring nurses to be adaptable and efficient. Some common responsibilities in this setting include:
- Assessing and monitoring patients’ conditions
- Administering medications and treatments
- Assisting with procedures or surgeries
- Collaborating with physicians and other healthcare professionals
- Educating patients and their families
Clinics
In clinics, nurses provide care in outpatient settings and often specialize in specific areas, such as primary care, women’s health, or occupational health. Clinic nurses may have more regular working hours than hospital nurses, as clinics typically have predetermined operating hours. Duties in a clinic setting can include:
- Conducting health assessments
- Providing routine care and health maintenance
- Assisting with procedures and diagnostic tests
- Collaborating with physicians and other healthcare professionals
- Educating patients about their conditions and promoting healthy habits
Community Health Settings
Nurses in community health settings focus on promoting health and preventing illness within specific populations. They often work in schools, community centers, or public health departments. These nurses play a crucial role in addressing healthcare disparities and improving the overall health of the community. Key responsibilities in this setting include:
- Health promotion and disease prevention
- Immunizations and health screenings
- Identifying and addressing health risks within the community
- Coordinating care with other healthcare providers and social services
- Providing education and resources to improve community health
Overall, nurses have diverse work environments to choose from, each providing unique opportunities to make a difference in the lives of patients and their families. By understanding the various settings, nurses can determine which environment best aligns with their individual career goals and passions.
The Nursing Process
The nursing process is a crucial aspect of nursing practice, ensuring optimal patient care and outcomes. This systematic approach is divided into four main components: Assessment, Planning, Implementation, and Evaluation.
Assessment
During the assessment phase, nurses carefully observe and gather data on patients’ health conditions, both through subjective and objective measures. This includes taking patient histories, performing physical examinations, and obtaining vital signs. Nurses also review data from lab results, imaging studies, and consult with other healthcare professionals to gain a comprehensive understanding of the patient’s health status. The assessment phase is essential for identifying any real or potential health problems that patients may be experiencing or may encounter in the future.
Planning
Once the assessment is complete, nurses use the information to create an individualized nursing care plan for the patient. This plan should outline the specific actions needed to meet the patient’s unique health needs. Goals should be established, both short-term and long-term, keeping in mind the expected outcomes associated with achieving these goals. The nursing plan should also prioritize the needs of the patient, addressing the most critical issues first.
Implementation
With the nursing care plan in place, the implementation phase begins. During this stage, nurses carry out the interventions outlined in the plan, working closely with other healthcare professionals to ensure seamless collaboration and coordination of care. Interventions may include administering medications, performing treatments, providing education, and offering emotional support. Nurses need to be vigilant during the implementation phase, being prepared to adjust the care plan as needed based on the patient’s response to the interventions.
Evaluation
Lastly, the evaluation phase involves continuously monitoring the patient’s status and assessing the effectiveness of the nursing care delivered. By revisiting the nursing care plan and comparing it with the actual outcomes, nurses can determine whether the interventions have been successful or if adjustments need to be made. If further interventions are necessary, the nurse should update the care plan and continue the process of implementation and evaluation until the desired outcomes are achieved.
The nursing process is an integral part of a nurse’s practice, providing a structured and effective approach to delivering patient care. By following the steps of assessment, planning, implementation, and evaluation, nurses can ensure they are meeting the unique needs of their patients and ultimately promoting optimal health outcomes.
Challenges in Nursing

Shift Work
Nurses often work long shifts that can range from 8 to 12 hours. These shifts can be physically and mentally taxing, leading to burnout. In addition, nurses must also adapt to rotating shifts, which can disrupt their sleep patterns and affect their overall well-being. To manage shift work challenges, nurses can employ self-care techniques, establish a regular sleep schedule when possible, and seek assistance from colleagues if needed.
Emotional Stress
Nursing is an emotionally demanding profession, as they frequently deal with patients experiencing end-of-life care and high-stress situations. The emotional stress can be exacerbated by the fact that nurses today are more specialized than ever; they are not easily replaceable and often bear additional responsibilities (source). Nurses should remember that it’s natural to feel emotional strain while working and can benefit from seeking support from colleagues or engaging in stress-reducing activities, such as exercise or meditation.
Physical Demands
Apart from long hours, nursing is a highly physical profession, involving lifting, moving, and supporting patients. The following are some common physical demands faced by nurses:
- Heavy lifting: Nurses may need to lift or transfer patients, which requires strength and proper body mechanics.
- Standing for long periods: Long hours on their feet can lead to leg and foot pain or fatigue.
- Repetitive movements: Nurses often perform similar actions (e.g., bending, reaching) multiple times daily, potentially causing strain or injury.
By practicing proper body mechanics, nurses can reduce the physical strain associated with their job. Additionally, maintaining a healthy lifestyle with regular exercise, stretches, and a balanced diet can help manage the physical demands of nursing.
Impact on Patient Outcomes
Quality of Care
Nursing care has a significant impact on the quality of care provided to patients. Research shows a modest evidence base for a link between missed care and patient outcomes, generated mostly from nurse and patient self-reported data. High-quality nursing care can lead to improved health status for patients. In a study comparing nurse case management to usual care, patients in the nurse case management group were more than twice as likely to report improvement in health status.
Some key aspects of quality of care impacted by nursing include:
- Patient safety: Nurses play a crucial role in ensuring that patients are safe during their stay in healthcare facilities. They monitor vital signs, administer medications, and track any changes in patients’ conditions.
- Disease management: Nurses are often responsible for managing patients’ long-term conditions, such as diabetes or high blood pressure, ensuring that patients receive appropriate care and treatment.
- Care coordination: Nurses act as a link between patients, their families, and other healthcare professionals, contributing to a well-coordinated care plan.
Patient Satisfaction
Nurses have a significant influence on patient satisfaction. They can affect whether a patient feels respected and cared for during treatment. Patients often spend more time with nurses than any other healthcare professional, so the quality of nursing care directly impacts their overall experience. According to the American Nurses Association, nurses excel in practicing patient empathy and attending to patients’ physical needs without compromising emotional support.
Factors contributing to patient satisfaction through nursing care include:
- Communication: Nurses who effectively communicate with patients and families can help alleviate fears and improve understanding of the treatment plan.
- Empathy and compassion: Nurses who display empathy and compassion make patients feel cared for and supported during their healthcare experience.
- Timeliness of care: Prompt attention to patients’ needs by nurses can greatly enhance their satisfaction with the healthcare system.
Healthcare Cost Management
Efficient and effective nursing care can help in managing healthcare costs. Proper nursing interventions can reduce the length of hospital stays and readmission rates, leading to overall cost savings for both patients and healthcare providers. Registered nurses (RNs) working in primary care interdisciplinary teams have shown positive contributions towards patient-level outcomes, further highlighting the importance of their role in healthcare cost management.
Strategies that help in cost management including:
- Preventing Hospital-Acquired Infections: By following strict infection control protocols and maintaining a clean environment, nurses can reduce the risk of patients acquiring infections during their hospital stay.
- Early intervention and discharge planning: Nurses play a crucial role in identifying patients’ needs for post-discharge care and coordinating with other healthcare providers to facilitate a timely and safe discharge.
- Utilizing evidence-based practices: Nurses who use evidence-based practices can help optimize patient outcomes and ensure that healthcare resources are used responsibly.
Future of Nursing

Technological Advancements
The nursing profession is constantly evolving as new technologies are developed and integrated into healthcare. Nurses are expected to adapt to the use of medical technology for diagnosis, treatment, and monitoring of patients. Some examples of advancements that may influence nursing include telehealth, robotics, artificial intelligence, and electronic health records. These innovations not only help streamline processes but also improve patient care outcomes.
Policy and Healthcare Reform
With the increasing focus on healthcare reform and policy changes, nurses have a critical role in demonstrating their value and importance in the healthcare system. Nurses need to be actively involved in these discussions, advocating for equitable policies that support their profession and improve patient care. Future nurses may be required to handle increased responsibilities due to changes in healthcare systems and an emphasis on health equity.
Nursing Education Trends
In order to meet the demands of the ever-evolving healthcare landscape, nursing education programs must adapt to changes in technology, policy, and patient populations. This includes expanding clinical exposure, addressing diversity within the nursing workforce, and empowering nurses with the necessary skills and knowledge. There is also a growing emphasis on interdisciplinary learning, with programs focusing more on collaboration between healthcare professionals to improve patient outcomes. According to the National Academy of Medicine, there will be an increased focus on higher education and specialization in the coming years.








[…] activation of a code blue, the medical team springs into action with a set of critical tasks. First, they rush to the patient’s […]
[…] (National Council Licensure Examination) is a crucial step for African nurses who wish to practice nursing in the United States. It is a standardized examination that assesses the competencies required […]
[…] regulations, but with persistence and dedication, you can achieve your American dream of working as a nurse in the United […]
[…] Nursing is a rewarding career, both in terms of personal satisfaction and financial compensation. Salaries for nurses can vary widely across the United States, with certain states offering significantly higher pay than others. This article will explore the top 10 highest paying US states for nurses, giving you insights into where you could potentially earn the most as a healthcare professional. […]